1. Understand What Spider Veins Are
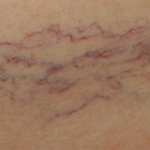
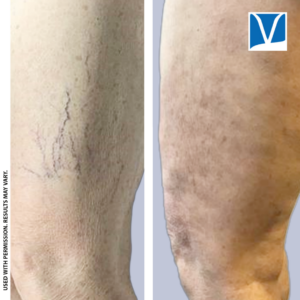
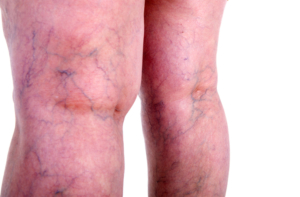
Spider veins are small blue or red veins at the skin’s surface. They are also known as telangiectasias and are most commonly seen on the legs and face. They can range from less than 1 mm to 4 mm in size. Most, but not all, are considered benign and are generally treated for cosmetic appearance purposes.
Sometimes, however, they are the “tip of the iceberg” so to speak. This means they are a manifestation of deeper vein issues such as chronic venous insufficiency. They usually arise due to high pressure in the underlying veins, which dilates the venules so they are visible.
Generally, spider veins are considered benign if they do not hurt, bleed, or throb. However, if you do experience these complications, there is usually additional venous insufficiency that you are not seeing. Occasionally, some patients can experience bleeding spider veins. When this occurs in the legs, especially around the ankle, the bleeding can be quite severe due to the high pressure from the underlying chronic venous insufficiency.
- Spider Veins
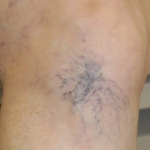
- Spider Veins
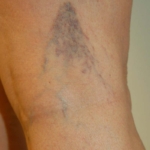
- Spider Vein with Reticulars
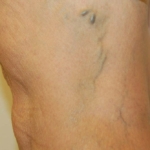
- Medium Veins
2. Learn Which Treatments Work and Which Do Not
There are a number of treatment options available including sclerotherapy (liquid or foam), surface laser treatments, and compression therapy. Graded compression hose can help reduce the symptoms such as throbbing, burning, aching and stinging. Surface laser or light-based treatments are an option, especially for the face. For the legs, in general, sclerotherapy is the mainstay of treatment.
Sclerotherapy is a procedure where inject veins with an FDA approved medication that is intended to cause the veins to shrivel up and fade away. This is done in our office, usually over the course of several outpatient vein treatment sessions. There is no need for anesthesia, and patients generally walk out after the procedure and can immediately return to regular activities. Usually, graded compression hose are used for a short period of time to compress the small veins while they are healing after sclerotherapy.
Sclerotherapy has been around for many years, and there are over 1 million sclerotherapy sessions yearly around the world to treat leg spider veins. Topical creams and indigestible pills generally cannot make spider veins fade away.
3. Recognize Your Reasons to Treat Spider Veins
Patients presenting for spider vein treatments generally fall into 2 categories. Most are simply interested in treating them for cosmetic purposes. The veins don’t hurt or ache, these patients report, they just don’t like how they look. This is considered cosmetic, and thus, not covered by most insurance companies. The treatment prices are generally reasonable, which allows many patients to pursue treatment for this reason.
Other patients are interested in having them treated for medical purposes. These patients often complain of burning, stinging, aching, or at times bleeding from their spider veins. This generally requires a more extensive medical work up to better understand the patient’s overall cardiovascular health and underlying venous function. Typically, most of these patients suffer from chronic venous insufficiency (also known as varicose veins). These patients can be treated with approaches like radiofrequency ablation of the greater saphenous vein (Closurefast), endovenous laser therapy, Venaseal, or Varithena polidocanol endovenous microfoam.
If you are not sure which category fits you, a simple evaluation by a vein specialist can usually sort this out in an initial consultation.
4. Develop a Treatment Plan With An Expert
Patients seeking treatment should see a vein specialist who is experienced not only in techniques such as sclerotherapy, but also in diagnosing and treating the entire spectrum of venous disorders so they can help you choose the optimal treatment plan. This usually starts with a consultation where the care provider examines your legs. At this time they also take a detailed medical history, especially focusing on your venous history. They will be particularly interested if you have leg swelling, or a history of blood clots (deep venous thrombosis or superficial venous thrombosis).
When significant venous insufficiency is suspected, they will often order a lower extremity venous ultrasound. This helps map out the normal and varicose veins. When it is simply spider veins and the primary reason to treat them is cosmetic, one can often proceed without a venous ultrasound directly to sclerotherapy treatment sessions.
When one has indications to evaluate the veins with a venous ultrasound and significant venous insufficiency is found in the veins below the skin (like the greater saphenous vein and its branches), then treatment plans may be more comprehensive to include approaches like radiofrequency ablation of the greater saphenous vein (Closurefast), endovenous laser therapy, Venaseal or Varithena polidocanol endovenous microfoam. Depending on the indications and findings, these treatments are covered by most insurance companies as being medically necessary.
5. Get Appropriate and Complete Treatment
 Appropriate treatment varies from patient to patient, but requires estimating the total number of treatment sessions needed, and making sure to treat the source feeder veins during these sessions. When treating spider veins, it is important to sort out with the provider how many sessions will be needed. If it is just one focal area, then one session may be sufficient. But when it is both legs, above and below the knees, and the front, back, and sides of the legs, it is not uncommon for many sessions to be required to achieve the best results.
Appropriate treatment varies from patient to patient, but requires estimating the total number of treatment sessions needed, and making sure to treat the source feeder veins during these sessions. When treating spider veins, it is important to sort out with the provider how many sessions will be needed. If it is just one focal area, then one session may be sufficient. But when it is both legs, above and below the knees, and the front, back, and sides of the legs, it is not uncommon for many sessions to be required to achieve the best results.
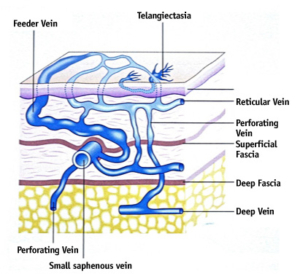
It is also important that the provider treats the “feeder” veins, known as reticular veins, otherwise the spider veins may take longer to fade away and may return quicker. Most experienced sclerotherapists are good at identifying and treating the feeder reticular veins, as well as making sure their patients have reasonable expectations about how many sessions will be needed to achieve optimal results.
6. Understand Expectations for Outcomes and Recurrence
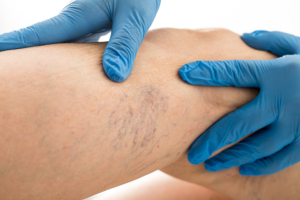 Treatment of spider veins with sclerotherapy takes time for optimal results. Often the veins darken a bit (showing), or can have a blush appearance while they are healing. Sometimes there is trapped coagulated blood in the veins that needs to be treated to make the color fade faster. This can take weeks, or sometimes months to fade, depending on the patient and the extent of treatments required.
Treatment of spider veins with sclerotherapy takes time for optimal results. Often the veins darken a bit (showing), or can have a blush appearance while they are healing. Sometimes there is trapped coagulated blood in the veins that needs to be treated to make the color fade faster. This can take weeks, or sometimes months to fade, depending on the patient and the extent of treatments required.
It is important for the patient and provider to discuss these expectations in advance so everyone agrees on what to expect. Photos are usually taken before each session so the patient can track their progress over the course of recovery. Long-term, spider veins can return. Many patients will schedule occasional “maintenance” sessions of sclerotherapy in the ensuing years to stay on top of the situation after their initial treatment.
Are you ready to address your spider veins?
If you are interested in learning more about varicose veins treatment options, simply fill out our Online Appointment Request Form or call any of our clinics in Northwest Portland , Tigard, Happy Valley, Hillsboro or Bend, Oregon.