Sclerotherapy is the most common procedure used to treat spider veins in the legs. Sclerotherapy involves the sequential injection of a medical solution into various points along the spider veins with a FDA approved solutions. This causes an irritation of the inside of the spider veins, leading them to shrivel up and fade away over time.
Sclerotherapy for Spider Veins
This procedure can be done for spider veins, called visual sclerotherapy, or can be used to treat the larger veins under the skin, in which we use ultrasound guidance.
When used in conjunction with ultrasound, it is referred to as ultrasound guided sclerotherapy (USGST). With ultrasound guidance, the ultrasound helps us identify the vein under the skin and track the location to the key target veins needed for the optimal results. The sclerotherapy agent can be left in liquid form, or be prepared as a foam. Foam sclerotherapy is particularly useful in conjunction with ultrasound for larger veins.
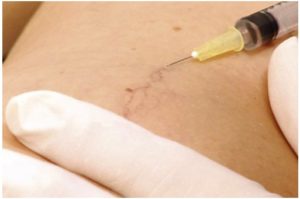
In the distant past, some doctors used hypertonic saline, also known as salt injections for sclerotherapy. Today the two most common agents used in modern sclerotherapy are sodium tetradecyl sulfate (Sotradecol) and polidocanol (Asclera). Hypertonic saline is simply a saline (salt) concentrate solution which irritates the tiny veins and subsequently closes them. It was also very inexpensive which meant that physicians who use it were able to charge a little less for their services.
The most important disadvantage of hypertonic saline was that it was very painful when injected. To help ease the pain, physicians sometimes mixed lidocaine in the solution or gave their patients Valium or a pain reliever, but this rarely made the burning go away entirely. Ulceration at the injection site was also not uncommon. For these reasons, we do not use hypertonic saline in our practice. (nor do most modern vein practices).
There are two modern alternatives: sodium tetradecyl sulfate (trade name Sotradecol) and polidocanol (trade name Asclera). Both are very similar to one another. We use both in our practice. While these solutions are more expensive, they provide a safer, more effective and less painful alternative to hypertonic saline as used in the old days.
Both Sotradecol and Asclera are medical grade detergent-like solutions that work by irritating the cells of the inner lining of the vein, known as endothelial cells. After injection spider vein essentially seal shut, close down and fade away over time. In part this works by causing clotting of the tiny spider veins leaving them to eventually disappear as blood reroutes to other healthy veins. The results are very similar between Sotradecol and Asclera. Both Sotradecol and Asclera can be used in various concentrations, depending on the size, locations and treatment goals.
Developing a Spider Vein Sclerotherapy Plan
Its important to develop a comprehensive treatment program before having sclerotherapy. We always meet with patients and evaluate the extent of treatment sessions needed. A session is one visit where the veins are treated. There are usually multiple tiny injections of the spider veins per session.
In sclerotherapy, the needles are very small and this is generally well tolerated by patients. Some patients simply need a focal area treated on one leg, and others need multiple treatments on both legs. In the initial evaluation a treatment plan is agreed to in terms of the expected number of treatment sessions needed to attempt to achieve the optimal results in spider vein clearance. We advise patients were a thigh high compression stocking for a week after each treatment session. This helps to compress the veins and speed optimal cosmetic results. Most patients can go right back to their usual activities.
The Sclerotherapy Procedure
Sclerotherapy is an effective spider vein treatment that does not require anesthesia and is typically performed in our office. The procedure takes about 15 to 30 minutes, but the exact length of time depends on the size of the area and the number of veins being treated. Depending on its size, a single vein may have to be injected more than once. Multiple veins may be injected during one treatment sessions.
Photographs of the target veins to be treated will be taken before the procedure. During the procedure, you’ll lie on your back with your legs slightly elevated. Your care provider will cleanse the area to be treated before inserting a solution into the targeted vein with a very tiny needle. You may experience some minor burning or stinging with the injection, but this generally quickly fades.
After the injections, your doctor will apply compression to keep blood out of the injected vein flat and disperse the solution. A compression stocking is placed while you are still laying down, and you are advised to wear it over night the first night, then every day for a week. After the first night, you can take off the compression stocking at night.
Patients can return to work the day after the procedure and can return to regular activity including exercise the next day after the procedure. We generally see the patient back in a week or two to assess outcomes in a scheduled follow up visit. We can use the photographs to track treatment progress when needed.
Potential Complications of Spider Vein Scelerotherapy
Like any medical intervention, there can be side effects or complications. Side effects are rare. The most important is the very rare incidence of an allergic reaction to the medication. Also rare are complications such as superficial or deep vein clots, infection or bleeding. However there are some side effects that are fairly common and must be discussed and understood in advance of the treatments. This includes hyperpigmentation, also known as staining or shadowing. This is where the treated vein becomes darker for a period of time. This happens from blood trapped in the treated vein. It generally fades with time. In some cases it takes weeks, but in others months and up to a year are needed for this to fade. Telangetatic matting can occur. This is a blush appearance in the area of treatment where tiny blood vessels form in response to the inflammation from the treatment. This usually fades with time as well. Sometimes this persists if there are surrounding reticular veins feeding the area. In that case, more sclerotherapy may be needed to obtain clearance faster. Very rarely an area of skin can become necrotic, known as a sclerotherapy induced skin ulcer. These heal with time. In other cases, skin laser or IPL can be helpful in clearing the blush. Rarely a patient will develop a migraine headache, cough or feel faint after a treatment session. This usually passes quickly.
As mentioned, occasionally there is trapped blood in the veins after sclerotherapy. This can become inflamed, and thus red, warm and tender. This is not unexpected. We check for these on follow up. Generally, this can be quickly treated in the office in follow up to help speed recovery.
Frequently Asked QuestionsSclerotherapy
-
-
Why do some spider vein treatments take so long to produce results?
We treat the veins, we do not remove them. After spider vein treatment, the body has to break down veins in a healing process where they fade away with time. Results are evident right away, but shadowing in darker veins can take months or longer to fade. However, patient satisfaction on sclerotherapy results is generally good when the patient understands this process and engages in the full treatment plan through multiple visits and follow up.
-
How long will it take for veins to disappear after sclerotherapy?
Every patient is different, but most see results from sclerotherapy right away. However, most patients also require multiple treatment sessions to achieve the results they are looking for, and it may take months for the veins to fade away after treatment.
-
Can you drink alcohol after sclerotherapy?
Alcohol is not specifically prohibited after sclerotherapy or any vein treatment, but as usual, it is always best to drink in moderation rather than excess.
-
Is foam sclerotherapy painful?
Sclerotherapy treatments are done in the office and are generally well tolerated by the patients. There is the sensation of needle sticks from the small needle used to inject the medication, and/or a bit of burn when the medicine goes in, but this generally fades quickly. Most feel the discomfort is gone once they get up and get ready to leave the office.
-
What should patients avoid after sclerotherapy?
It’s important to take it easy the first night after sclerotherapy. Exercise like running, jumping, dancing, etc should be avoided, but can be resumed starting the next day.
-
Can you walk after sclerotherapy?
Yes - walking is encouraged. In most cases we ask that patients take it easy the first night after sclerotherapy, but most can resume normal activities starting the next day.
-
What is the fastest way to recover from sclerotherapy?
The recovery is the same after most office-based vein procedures. There can be some tenderness along the treated veins which may take a few weeks or longer to fully resolve, but in most cases, patients can resume their normal activities the next day.
-
About Inovia Vein Specialty Centers
At Inovia Vein Specialty Centers we are leading vein doctors who specialize in caring for patients with venous disorders such as varicose veins, deep venous thrombosis, and venous stasis ulcers. Founded in 2006, we have specialty vein clinics across the Pacific Northwest. Call to set up a consultation to learn more about your treatment options.



