Any vein can develop a blood clot. Blood clots in the deep veins are called deep vein thrombosis, or DVT. Blood clots in the superficial veins are called superficial vein thrombophlebitis…or SVT. Commonly, however, it is known simply superficial vein phlebitis.
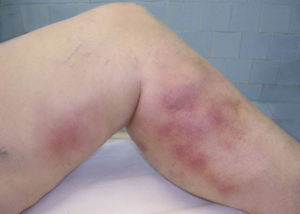 We are often contacted from patients or their referring physicians for treatment for superficial vein phlebitis. These most commonly occur in varicose veins in the leg, but any superficial vein can develop a clot.
We are often contacted from patients or their referring physicians for treatment for superficial vein phlebitis. These most commonly occur in varicose veins in the leg, but any superficial vein can develop a clot.
Clots in the superficial varicose veins of the legs can be a benign and self-limited problem. However, when the blood clot occurs in the larger superficial varicose veins, it can spread into the deep veins of the leg, referred to as a deep vein thrombosis (DVT) and potentially break off and move through the heart to the lungs, called a pulmonary embolism…or PE. Therefore superficial vein phlebitis is considered a serious medical condition.
Generally the treatment of superficial vein phlebitis is to prevent spread to the deeper veins. Sometimes this requires a blood thinner. Patients should be seen by a qualified healthcare provider who can help determine the extent of the clot (usually with Ultrasound), then develop a short and long term treatment plan.
Findings on Physical Exam
Clots in the superficial veins most frequently occur in the legs in association with varicose veins. When a blood clot occurs in the arm, it is general associated with an IV placement.
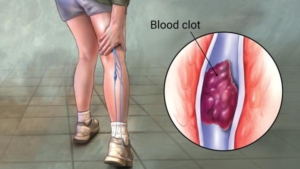
Phlebitis refers to acute inflammation of the vein, and thrombo- refers to a clot in the vein. Clot itself is highly inflammatory.
When a person has superficial vein phlebitis, they will often have pain, tenderness, redness and what feels like a cord under the skin. This can be quite painful. This can look like an infection, although most are not infected with bacteria. It can also look like a deep vein thrombosis.
Ninety percent of cases of phlebitis occur in people with pre-existing varicose veins. When varicose veins are not present, and the patient has not had a recent IV, then medical causes can be considered as well.
Clinical Course and Complications of Superficial Vein Phlebitis
Most clinical presentations are uncomplicated with typical findings of tenderness, firm skin, pain, and redness along the varicose vein. The degree of inflammation varies depending on the length of the vein affected. There is often a cord like feeling under the skin that feels like a small rope, with redness over this cord. Low-grade fever may be present in uncomplicated superficial thrombophlebitis, but high fever should increase suspicion for infection in the superficial thrombophlebitis.
Complications of superficial vein phlebitis can also occur. The biggest concern in the short term is spread from the superficial veins to the deep veins. Long term, the phlebitis can re-occur. Rarely, infection can arise in the clotted veins, which is associated with high fever, and redness that extends well past the affected vein. In these patients, IV antibiotics are required, and possibly removal of the infected vein.
The diagnosis of phlebitis and thrombosis of the lower extremity superficial veins is usually clinically apparent based upon the patient’s complaints and physical examination as described above, especially in patients with known risk factors.
The need for duplex ultrasound or further evaluation with laboratory or other studies depends upon the clinical scenario. Most feel that duplex examination is essential for patients with suspected superficial vein thrombosis due to the high rate of concurrent deep vein thrombosis (DVT), as well as to accurately make the diagnosis and define the location of the clot so the patient can be reevaluated if the symptoms worsen.
Treatment of Phlebitis
Treatment differs depending upon whether the thrombosis affects larger superficial varicose veins, as well as the greater, or small saphenous veins, and how close the clot is to the junctions with the deeper veins. This can be determined by ultrasound. Also if the condition seems to be worsening, that can mandate a different treatment approach.
For uncomplicated disease, treatment is primarily aimed at alleviating symptoms and preventing spread of clot into the deep venous system. This is done with compression hose, exercise, leg elevation and non steroidal anti-inflammatory medications.
Usually a close follow up is planned, and follow up ultrasound is performed until it is clear the condition has resolved. In some cases, anticoagulant medication is used stop the clotting process in an effort to prevent spread of the clot to the deeper veins. This can include drugs like Xarelto and Eliquis, or shots like Low Molecular Heparin (Lovenox or Arixtra).
You and your care provider can discuss if anticoagulant medications are indicated, and if so, for how long. Long term if the condition was triggered by large varicose veins, then you might consider discussing if your varicose veins should be treated with procedures like Closurefast, Venaseal, Varithena, or some form of sclerotherapy to help reduce the risk of recurrence in the future.
Generally, if you think you might have superficial vein phlebitis you should seek medical input, especially if the veins are red, hot, tender and hard and if the condition seems to be worsening.
Oregon’s Leading Vein Care Specialists
At Inovia Vein Specialty Centers we specialize in caring for patients with venous disorders such as varicose veins, deep venous thrombosis, and venous stasis ulcers.
If you are interested in learning more about vein treatment options, simply fill out our Online Appointment Request Form or call any of our clinics in Northwest Portland , Tigard, Happy Valley or Bend, Oregon.
